COVID-19 has changed the way we live. For a few, like Annie Cheng, it’s also practically changed where they live.
“I have a completely different lifestyle now,” she said. “Pretty much the lab is my home.”
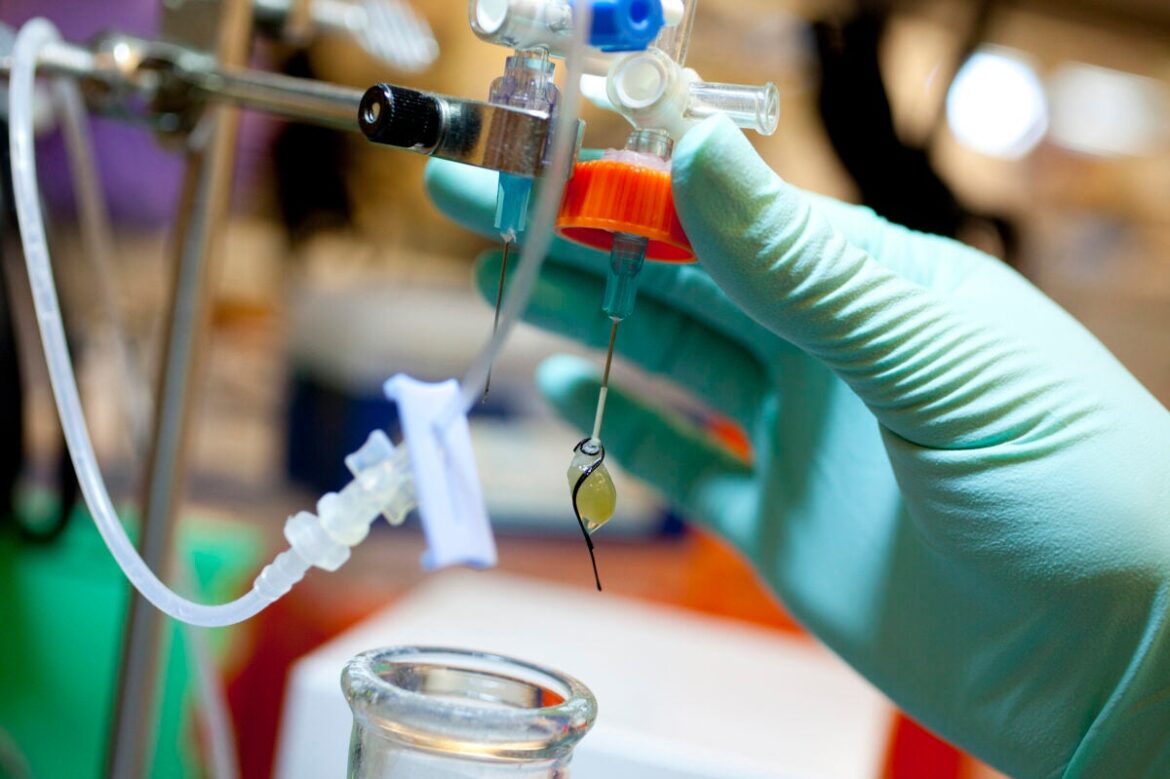
Cheng, the lead technologist at Beth Israel Deaconess Medical Center’s molecular diagnostics lab, is among those toiling to transform it from a regular 7 a.m.‒5 p.m., five-day-a-week operation into one of New England’s foremost hospital-based testing centers for SARS-CoV-2, the virus that causes COVID-19.
The lab has super-charged its capacity. It recently performed 1,000 tests in a day and can do as many as 1,500, an entire season’s worth of flu diagnostics. This has meant longer hours for everyone, new testing machines, and redesigned procedures to keep workers safe. But the real game-changer has been the influx of skilled volunteers from Beth Israel’s research labs, which were closed after social-distancing edicts went into effect.
“Ordinarily, we have a small number of people in our clinical lab who do this [testing] work,” said Jeffrey Saffitz, chair of Beth Israel’s Pathology Department and Mallinckrodt Professor of Pathology at Harvard Medical School (HMS). “All of the basic science laboratories at Harvard Medical School and its hospitals have been closed down, so we have this large population of research techs and postdocs who run PCR machines all the time in a research setting. We put out a call and we were gratified to have a great response. It’s a story where our community of smart, incredibly committed people will do whatever it takes to stem this terrible tragedy.”
The scramble began in mid-March, when the government allowed hospital labs to begin their own testing for SARS-CoV-2 instead of sending samples to centralized government facilities for results. The change came as U.S. disease numbers skyrocketed and what had been insistent calls for increased testing capacity rose to a shout.
Beth Israel has two main labs that do its clinical testing. Officials decided that one, the molecular diagnostics lab, equipped with high-volume machines, would handle the COVID tests. The lab, however, was initially hamstrung by a lack of test kits that would allow its machines to check samples for COVID. The shortage was met by Aldatu Biosciences, a startup with roots in Harvard’s i-lab and Pagliuca Life Lab. Soon afterward, supplies from Abbott Laboratories, which makes the machines, began to flow.